Thyroid Goiter: The Diagnosis and Treatment of Thyroid Goiters
What is a Thyroid Goiter?
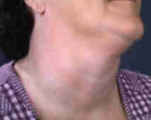
Thyroid goiter is a condition where there is an abnormal enlargement of your thyroid gland. The photo here shows how many thyroid goiters look, which is like the neck is swolen and fat. When you touch it, you can tell it isn't fat since it is firm and doesn't move much. Most thyroid goiters are painless, but they may produce symptoms due to their size itself. The most common symptom from a thyroid goiter is a lump in the neck. Other symptoms from a large thyroid goiter may include a sense of a lump in the throat, difficultly swallowing, difficulty breathing and even in extreme cases, voice changes and even vocal cord paralysis.
World wide, the most common cause of thyroid goiter is in locations where iodine in the diet is low or non-existent. This was similarly the case in the United States where thyroid goiter was commonplace until the contemporary iodination of table salt. Since then, the incidence of thyroid goiters have drastically been reduced in the United States.
Today, in the United States, thyroid goiter is more commonly associated with too much production of thyroid hormone (hyperthyroidism), too little production of thyroid hormone (hypothyroidism), or multiple nodules within the thyroid gland itself (mulitnodular goiter).
There are two autoimmune conditions (where the body recognizes something abnormal about itself and produces an antibody against this self part) that can be causes of thyroid goiter.
Hashimoto's thyroiditis.
- Patients have diffuse enlargement of their thyroid gland during the early stages of their autoimmune condition.
- The disease can be diagnosed by blood tests that show antibodies to the protein produced by the thyroid gland called thyroglobulin.
- Ultrasound may show diffuse vascularity of the thyroid gland and pseudonodules of the thyroid. Pseudonodules are indiscreet nodules which may be an artifact of the disease and may be present on one ultrasound and in followup ultrasounds the pseudonodule may no longer be found.
Grave's disease.
- Produces a serious medical condition of too high thyroid hormone levels (hyperthyroidism).
- Caused by a production of a protein called thyroid stimulating immunoglobulin
- Can be effectively found in the blood using routine testing.
- Attaches to the thyroid gland
- Causes the thyroid to overproduce thyroid hormone
- Causes the thyroid gland to enlarge.
Goiter Guru on YouTube
Dr. Rashmi Roy, Senior Surgeon at the Clayman Thyroid Center & Hospital for Endorine Surgery, has an entire YouTube channel dedicated to thyroid goiters. Dr. Roy operates on a significant number of patients with thyroid goiters, many of whom other surgeons refuse because of their complexities. Check out the Goiter Guru YouTube Channel here.Symptoms of Thyroid Goiters
Most thyroid goiters don't cause symptoms, but they will if the goiter continues to grow. In fact, small thyroid goiters may more commonly be detected by routine examination of the patient's neck by a doctor or by some type of screening x-ray or scan for some other reason. The symptoms occur as the goiter becomes big enough that it presses on other structures in the neck.
Larger thyroid goiters most commonly produce symptoms of
- A mass or lump in the neck.
- Uncomfortable pressure sensation on the breathing tube (trachea)
- A sense of feeling like you need to swallow something or difficulty swallowing
- Excess production of the thyroid hormone, thyroxine which include:
- Unexplained weight loss
- Heat intolerance
- Tremor
- Nervousness
- Rapid or irregular heart rate
What Are The Potential Causes of Thyroid Goiter?
Several conditions may cause or predispose to the development of thyroid nodules including:
- Iodine deficiency
- Diets deficient in iodine can predispose individuals for the development of thyroid goiters. Portions of the world continue to lack iodine in their diets however in the United States, the presence of iodine in our daily diets makes this an unlikely cause for thyroid nodules.
- Overgrowth of normal thyroid tissue
- The reason why these thyroid goiters occur is not well understood. This is a condition called follicular hyperplasia (the follicular cell is a normal appearing thyroid cell). Both follicular hyperplasia and follicular adenomas are clearly not cancerous and are not worrisome and do not require removal except if they are symptomatic due to their size.
- Thyroid cysts
- Thyroid cysts are fluid filled cavities caused by degenerating thyroid adenomas, congenital cysts, or overproduction of a fluid produced by the thyroid called colloid.
- Inflammatory diseases of the thyroid (called thyroiditis)
- Hashimoto's thyroiditis or Hashimoto's disease is a chronic inflammatory condition of the thyroid gland caused by an autoimmune event where the patient develops antibodies to thyroglobulin (a normal protein produced by the thyroid gland). Long standing Hashimoto's thyroiditis is frequently associated with decreased thyroid hormone production call hypothyroidism. Hashimoto's thyroiditis may also be associated with thyroid pseudo-nodule formation. These pseudo nodules are not concerning thyroid nodules. Pseudo nodules found on ultrasound in thyroiditis patients will come and go based upon unknown issues.
- Multinodular disease of the thyroid (also called Multinodular Goiter or just "Goiter"
- Multinodular goiter is a thyroid gland which contains multiple thyroid nodules. The cause of multinodular goiter is not known but in some instances there may be a strong family history of goiters. Multinodular goiters can be quite massive and extend throughout the neck and well into the chest cavity.
- Thyroid Cancer
- Although the likelihood that a thyroid nodule is a cancer is quite low, the following are associated with an increased malignant risk:
- Age less than 30 years of age
- Age greater than 50 years of age
- Men greater than women
- A positive family history of thyroid cancer
- A positive family history of other endocrine cancers
- A history of radiation exposure
- Larger thyroid nodules
- Vocal cord paralysis (hoarseness)
- Although the likelihood that a thyroid nodule is a cancer is quite low, the following are associated with an increased malignant risk:
What Is The Evaluation Of A Thyroid Goiter?
The following are a list of tests that are required in the evaluation of a patient with a Thyroid Goiter.
- Complete Medical History and Physical Examination
- Ultrasound
- Blood Tests
- TSH
- T3 and T4
- Thyroglobulin (we obtain but not all doctors do so)
- Thyroglobulin Antibody (we obtain because it lets us know if there is an underlying inflammatory condition of the thyroid)
- Thyroid Stimulating Immunoglobulin
- Laryngoscopy (looking at the voice box)
- Ultrasound with possible Fine Needle Aspiration guided (FNA)
Medical history and physical examination is required for all patients with a thyroid goiter
If there is a suspicion that you may have a thyroid goiter, your health care professional will want to know your complete medical history. You will be asked questions about your possible risk factors, symptoms, and any other health problems or concerns. If someone in your family has had a diagnosis of thyroid goiter, thyroid cancer or other endocrine cancers, these are important factors.
Your doctor will examine you to get more information about possible signs of thyroid goiter and other health problems. During the exam, the doctor will pay special attention to the size and firmness of your thyroid and any enlarged lymph nodes in your neck. Examination of your voice box is part of the physical examination obtained by the surgeon for any thyroid goiter. A small lighted microscope is used to look at the voice box to determine how the vocal cords of the voice box are functioning. Even though a patient does not report change in their voice does not insure that the vocal cords are working normally. A vocal cord that is paralyzed greatly increases the concern that a thyroid goiter may be hiding a thyroid cancer.
Thyroid Goiter: The Definitive Diagnosis of a Thyroid Goiter is Made by High Resolution Ultrasound Examination
- The diagnosis of thyroid goiter is made with a comprehensive ultrasound examination of the entire thyroid gland and neck lymph nodes. Ultrasound exposes you to no radiation whatsoever. It uses sound waves to look beneath the skin at the important structures of your neck. Needle biopsy is only indicated if there is a mass within the thyroid goiter which is suspicious for malignancy.
- Ultrasound is used to see the thyroid gland and the lymph node of the neck. During biopsy, the ultrasound helps make sure they are getting FNA samples from the right areas.
- FNA is generally done on all thyroid nodules that are big enough to be felt. This means that they are larger than about 1 centimeter (about 1/2 inch) across.
- FNA biopsies of swollen or abnormal appearing lymph nodes in the neck may be more informative than the thyroid nodule itself in obtaining a diagnosis.
- Cells from the suspicious area are removed without an incision or discomfort and looked at under a microscope.
- The process of obtaining this small sampling of cells is called fine needle aspiration (FNA) cytology.
- This type of biopsy can usually be done in your doctor's office or clinic.
- Before the biopsy, local anesthesia (numbing medicine) may be injected into the skin over the thyroid nodule.
- Your doctor will place a thin, hollow needle directly into any suspicious dominant nodules within the thyroid goiter to aspirate (take out) some cells and possibly a few drops of fluid into a syringe.
- The doctor usually repeats this 2 or 3 more times, taking samples from several areas of the nodule.
- The content of the needle and syringe are then placed on a glass slide and then the FNA samples are then sent to a lab, where they are looked at under a microscope by the expert Cytologist to see if the cells look cancerous or benign.
- Cytology means looking at just the cells under the microscope.
- Thyroid cytology requires an expert physician (called a Cytologist) trained specifically in the diagnosis of thyroid nodules and thyroid cancers!!!
- Unfortunately, the diagnosis of thyroid nodules are frequently misinterpreted by unskilled or inexperienced Cytologists.
- Bleeding at the biopsy site is very rare except in people with bleeding disorders. Even when this occurs, the bleeding is almost always very self limited. Be sure to tell your doctor if you have problems with bleeding or are taking medicines that could affect bleeding, such as aspirin or blood thinners.
- Sometimes an FNA biopsy will need to be repeated because the samples didn't contain enough cells.
- Most FNA biopsies will show that the thyroid goiters are benign.
- Rarely, the FNA biopsy may come back as benign even though a diagnosis of a thyroid cancer is actually present.
Thyroid Goiter: When is a Radioiodine Scan Ordered?
If you have a thyroid goiter and your blood tests also demonstrate that your thyroid hormone level is too high (hyperthyroidism), this is the only instance that a radioiodine scan (thyroid scan) is indicated. In these cases, the thyroid stimulating hormone (TSH) will be very low and in cases of Grave's disease, the thyroid stimulating immunoglobulin will be very high. The thyroid goiter patient may or may not have recognized symptoms of their hyperthyroidism.
During the thyroid scan, the patient will be given a small amount of radioactive iodine in a pill and a special imaging camera is utilized to determine how much iodine is taken up by the thyroid gland and if the thyroid goiter takes up iodine throughout the thyroid gland or whether there is a single "hot" area in the thyroid , relative to the remainder of the thyroid gland (this is called a "hot nodule"). If a thyroid nodule has less iodine uptake than the rest of the thyroid gland, then the thyroid nodule is called a "cold nodule". In patients with multinodular goiter, frequently several of the nodules of the thyroid will be cystic and filled with fluid. These cystic areas of a multinodular goiter are expected to take up less iodine than the rest of the gland and appear "cold".
Hot nodules are almost always non-cancerous but the preferred management of hot nodules is frequently surgery since it is a clear, safe and 100% effective therapy for the hyperthyroidism.
Thyroid Goiter: When is a CT Scan ordered?
When physical examination and or ultrasound cannot completely determine how far the goiter actually goes, then a CT scan should be ordered. The CT scan will show areas that the thyroid goiter extends and prepare the expert thyroid surgeon their safe and effective approach to remove all of the goiter gland and spare all other structures. Even though a thyroid goiter may extend extensively below the sternum (breast bone) and go well into the chest, these goiters can almost routinely be removed through a relatively straight forward low collar incision in the lower neck. If your surgeon is telling you that they need to "split your chest" or "open your sternum", make sure that you have identified a highly experience thyroid surgeon. Again, such approaches are almost never actually required.
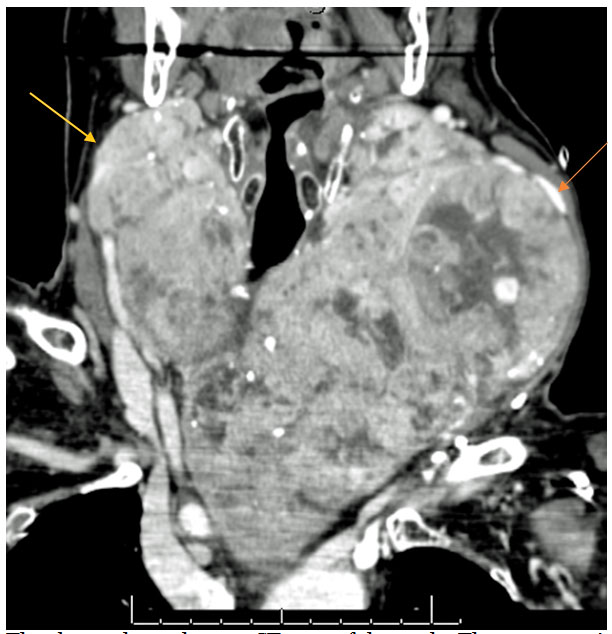 The above photo shows a CT scan of the neck. The arrows point to a thyroid goiter that essentially fills the entire neck and extends into the upper chest surrounded by the blood vessels leaving the heart and veins leading the return of blood to the heart. This requires is a straight forward surgery with a lower neck collar incision and leaving the hospital the next morning.
The above photo shows a CT scan of the neck. The arrows point to a thyroid goiter that essentially fills the entire neck and extends into the upper chest surrounded by the blood vessels leaving the heart and veins leading the return of blood to the heart. This requires is a straight forward surgery with a lower neck collar incision and leaving the hospital the next morning.
What Are The Treatments For Thyroid Goiter?
- Observation
- If the ultrasound with or without biopsy suggests that the patient has benign small thyroid goiter and there are little to no symptoms, the doctor may suggest simply watching the patient and the goiter. The duration of observation is however somewhat arbitrary. Observation usually implies repeating thyroid blood tests, ultrasound, and physical examination in approximately one year. If the thyroid goiter should increase in size or establish symptoms, another intervention may be indicated. Small thyroid goiters that don't change over a period of years may never require any treatment whatsoever.
- Thyroid Hormone Therapy
- If you have hypothyroidism (low thyroid hormone), your doctor will prescribe you thyroid hormone in the form of a pill or capsule. There are different types of thyroid hormone pills that doctors may prescribe to deal with low hormone levels. In theory, prescribing thyroid hormone can lower the thyroid stimulating hormone (TSH) production of the pituitary gland and thus decrease the stimulation to growth of thyroid tissue. In many instances, when patients have been hypothyroid, this may result in a decrease in the size of the thyroid goiter.
- If you have hyperthyroidism [high thyroid hormone and very low thyroid stimulating hormone (TSH)], your doctor will likely prescribe you a medication to control your hyperthyroidism. There are two medications which are commonly prescribed to control hyperthyroidism. The first is methimizole and the second is propthiouracil (PTU). These medications need to be prescribed by endocrinologists that understand how these medications work and potential side effects and complications from their use. These medications can be utilized to prepare you for:
- Radioactive iodine therapy
- Surgery
- Continued observation of your thyroid goiter
- If you have an inflammatory condition of your thyroid goiter, your doctor may prescribe you medications which treats inflammation. Both aspirin, corticosteroids (steroids), and non-steroidal anti-inflammatory medication may be prescribed for thyroid goiters associated with autoimmune or other inflammatory causes.
- Radioactive Iodine Therapy
- Used in circumstances where the thyroid goiter is associated with excess thyroid hormone production
- Taken orally
- RAI treatment frequently results in reduced size of the goiter
- Long term usually results in a need for thyroid hormone replacement lifelong
- Surgery
- Sometimes clearly thyroid goiters and multinodular goiters are managed with surgery. Some potential indications for removing thyroid goiters include:
- The thyroid goiter is large (producing a visible mass in the neck)
- The thyroid goiter is producing symptoms on the breathing tube or swallowing tube
- The thyroid goiter is producing excessive thyroid hormone
- Thyroid nodules which have Indeterminate or suspicious for cancer FNAs.
- Multinodular goiters producing symptoms
- A thyroid goiter which has progressed or remains symptomatic following RAI treatment
- Sometimes clearly thyroid goiters and multinodular goiters are managed with surgery. Some potential indications for removing thyroid goiters include: