Graves' Disease
- Most common cause of hyperthyroidism in the United States
- An autoimmune condition
- Diagnosed by detection of thyroid stimulating immunoglobulin (TSIB)
- TSI appears to have some ability to bind to the thyroid stimulating hormone (TSH) receptor thus producing the hyperthyroidism
- Effects women more commonly than men
- Appears to have some hereditary component
What Are the Symptoms Of Graves' Disease?
Early in the course of Graves' Disease, the symptoms may be similar to other conditions and may delay or confuse the diagnosis.
The following are a list of the more common symptoms of Graves' Disease:
- Unexplained weight loss
- Even though your appetite may be excessive
- Heat intolerance or excessive sweating
- Anxiety, Tremors, Restlessness
- Difficulty sleeping at night
- Nervousness
- Rapid or irregular heart rate, palpitations or chest pain
- Difficulty breathing or shortness of breath
- Goiter or thyroid mass
- Prominent buldging eyes
- Blurred vision, double vision
- Muscle weakness
- Change in menstrual periods
- Increased frequency of bowel movements
What Are The Physical Signs and Symptoms of Graves' Disease?
Untreated and undiagnosed Graves' disease may develop the following findings which will be readily appreciated by your skilled endocrinologist:
Thyroid Goiter - Graves' Disease will produce diffuse enlargement of the thyroid gland Called diffuse thyrotoxic goiter. Which may produce symptoms of:
- Difficulty swallowing
- Pressure
- Change in voice
- Tenderness
- Shortness of breath
- Change in vision
Graves' Disease Changes to the Eyes (called Graves' Opthalmopathy) - Changes to the eyes can be mild to severe
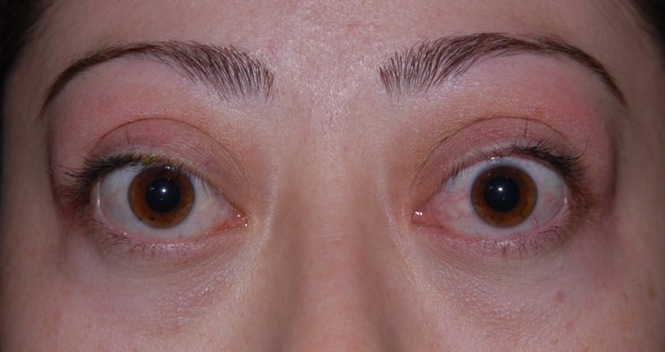 This picture is a woman with Grave’s Opthalmopathy. She is not making an effort to show her eyes to be big. Her eyes appear to be bulging because they are actually protruding out of her eye sockets. This does not reverse or go away following treatment. Early diagnosis and treatment can prevent Grave’s eye symptoms from developing.
This picture is a woman with Grave’s Opthalmopathy. She is not making an effort to show her eyes to be big. Her eyes appear to be bulging because they are actually protruding out of her eye sockets. This does not reverse or go away following treatment. Early diagnosis and treatment can prevent Grave’s eye symptoms from developing.
-
Mild eye symptoms
- Red
- Dry
- Excessive tearing
-
Severe eye symptoms
- Blurred vision
- Limited eye movement resulting in double vision
- Protruding of the eyes from their sockets
- Thickening of the skin of the lower leg (called pretibial myxedema)
- The skin lesions are patchy and red
What Causes Graves' Disease?
Graves' disease is an autoimmune disease where the body's immune system, for some reason, turns against a part or parts of the body. Although we know little about why this occurs, we do know that some patient's families clearly can have apparent predispositions to Graves' disease. As a result of this autoimmune event, patients with Graves' disease produce proteins called thyroid stimulating immunoglobulins. These immunoglobulins have the ability to link to a type of keyhole on the thyroid cells thyroid stimulating hormone (TSH) receptor just as TSH will do. In this way, the thyroid stimulating immunoglobulins push the thyroid cells to produce hormone in a continuous and unregulated fashion. In fact, there is no way to turn it off since the thyroid stimulating immunoglobulin production is not controlled in any way. The thyroid cells basically get tricked into producing more and more thyroid hormone thus producing hyperthyroidism.
Graves' Disease Diagnosis: How Is It Made?
The following are a list of tests that are required in the evaluation of a patient with a Graves' Disease.
- Complete Medical History and Physical Examination
- Ultrasound
- Blood Tests
- TSH
- T3 and T4
- Thyroglobulin (we obtain but not all doctors do so)
- Thyroglobulin Antibody (we obtain because it lets us know if there is an underlying inflammatory condition of the thyroid)
- Thyroid Stimulating Immunoglobulin
- Thyroid Peroxidase Antibody
- Laryngoscopy (looking at the voice box)
- Ultrasound with possible Fine Needle Aspiration guided (FNA)
- Radioactive Iodine Uptake and Scan
Medical history and physical examination is required for all patients with a potential diagnosis of Graves' Disease.
If there is a suspicion that you may have a Graves' Disease, your health care professional will want to know your complete medical history. You will be asked questions about your possible risk factors, symptoms, and any other health problems or concerns. If someone in your family has had a diagnosis of Graves' disease or other autoimmune disorders, these are important factors.
Your doctor will examine you to get more information about possible signs of thyroid goiter and other health problems. During the exam, the doctor will pay special attention to the size and firmness of your thyroid and any enlarged lymph nodes in your neck. Examination of your voice box is part of the physical examination obtained by the surgeon for any patient with Graves' disease. A small lighted microscope is used to look at the voice box to determine how the vocal cords of the voice box are functioning. Even though a patient does not report change in their voice does not insure that the vocal cords are working normally. A vocal cord that is paralyzed greatly increases the concern that a thyroid may be hiding a thyroid cancer.
Examination of your eyes may be required by a qualified ophthalmologist if you are having any visual symptoms.
Graves' disease: How is a Definitive Diagnosis Made?
- The diagnosis of Graves' disease is made with a comprehensive analysis of the blood including thyroid stimulating hormone (TSH), Free T4 levels and Free T3 levels. In most cases of Graves' disease the TSH level will be quite low consistent with a hyperthyroid condition. The pituitary gland which secretes TSH and stimulates thyroid tissue to produce thyroid hormone is trying to decrease the production of thyroid hormone. But this mechanism is failing to control for hyperthyroidism.
- The definitive diagnosis of Graves' disease is made with the detection of thyroid stimulating immunoglobulin (TSI). This is an antibody which can be measured in a simple blood sample. This antibody causes the thyroid cell to produce thyroid hormone by "tricking it" by grabbing on to the TSH keyhole of the cell which is the normal signal of the cell to produce hormone. The TSI also causes the complications of Graves' disease including the eye and skin symptoms.
- A blood test for Thyroid Peroxidase Antibodies (TPO) also supports a diagnosis of Graves' disease. This is another blood test that supports an autoimmune condition of the body finding the thyroid gland to be "abnormal". If you have these antibodies, it suggests the immune system is attacking the thyroid gland. However, nearly 5-10% of healthy individuals test positive for TPO without evidence of an autoimmune condition. Therefore the test does not define Graves' disease.
- Ultrasound is used to see the thyroid gland and the lymph nodes of the neck. In Graves' disease diffuse enlargement of the thyroid gland is anticipated with prominent numbers and sizes of blood vessels coming to and leaving the thyroid gland. Ultrasound exposes you to no radiation whatsoever. It uses sound waves to look beneath the skin at the important structures of your neck. Needle biopsy is only indicated if there is a mass within the thyroid goiter which is suspicious for malignancy.
- FNA is generally done on all thyroid nodules that are big enough to be felt. This means that they are larger than about 1 centimeter (about 1/2 inch) across. If you are already planning a thyroid surgery for Graves' disease, then biopsy of a nodule would not necessarily be indicated unless it would change the approach for your thyroid surgery.
- FNA biopsies of swollen or abnormal appearing lymph nodes in the neck may be more informative than the thyroid nodule itself in obtaining a diagnosis.
- Cells from the suspicious area are removed without an incision or discomfort and looked at under a microscope.
- The process of obtaining this small sampling of cells is called fine needle aspiration (FNA) cytology.
- This type of biopsy can usually be done in your doctor's office or clinic.
- Before the biopsy, local anesthesia (numbing medicine) may be injected into the skin over the thyroid nodule.
- Your doctor will place a thin, hollow needle directly into any suspicious dominant nodules within the thyroid goiter to aspirate (take out) some cells and possibly a few drops of fluid into a syringe.
- The doctor usually repeats this 2 or 3 more times, taking samples from several areas of the nodule.
- The content of the needle and syringe are then placed on a glass slide and then the FNA samples are then sent to a lab, where they are looked at under a microscope by the expert Cytologist to see if the cells look cancerous or benign.
- Cytology means looking at just the cells under the microscope.
- Thyroid cytology requires an expert physician (called a Cytologist) trained specifically in the diagnosis of thyroid nodules and thyroid cancers!!!
- Unfortunately, the diagnosis of thyroid nodules are frequently misinterpreted by unskilled or inexperienced Cytologists.
- Bleeding at the biopsy site is very rare except in people with bleeding disorders. Even when this occurs, the bleeding is almost always very self limited. Be sure to tell your doctor if you have problems with bleeding or are taking medicines that could affect bleeding, such as aspirin or blood thinners.
- Sometimes an FNA biopsy will need to be repeated because the samples didn't contain enough cells.
- Most ultrasounds for Graves' disease will show that the Graves' diseased thyroid glands are benign.
- Rarely, the FNA biopsy may come back as benign even though a diagnosis of a thyroid cancer is actually present.
Graves' Disease: What Does A Radioactive Iodine Scan Show?
If you possibly have Graves' disease and your blood tests also demonstrate that your thyroid hormone level is too high (hyperthyroidism), this is when a radioiodine scan (thyroid scan) is indicated. In these cases, the thyroid stimulating hormone (TSH) will be very low and in cases of Grave's disease, the thyroid stimulating immunoglobulin will be very high. The Graves' disease patient may or may not have recognized symptoms of their hyperthyroidism.
During the thyroid scan, the patient will be given a small amount of radioactive iodine in a pill and a special imaging camera is utilized to determine how much iodine is taken up by the thyroid gland and if the thyroid takes up iodine throughout the thyroid gland or whether there is a single "hot" area in the thyroid, relative to the remainder of the thyroid gland (this is called a "hot nodule"). A high uptake of iodine by the thyroid gland is suggestive of Graves' disease or hyperthyroidism. If a thyroid nodule has less iodine uptake than the rest of the thyroid gland, then the thyroid nodule is called a "cold nodule". In patients with multinodular goiter, frequently several of the nodules of the thyroid will be cystic and filled with fluid. These cystic areas of a multinodular thyroid are expected to take up less iodine than the rest of the gland and appear "cold".
Hot nodules are almost always non-cancerous but the preferred management of hot nodules is frequently surgery since it is a clear, safe and 100% effective therapy for the hyperthyroidism.
Graves' Disease: When is a CT or MRI Scan ordered?
If you are having symptoms from your eyes, your doctor may order a CT or MRI of the orbit and skull base in order to determine the impact of the Graves' disease upon the eye, eye muscles, orbital fat, and surrounding structures.
A comprehensive compilation of all physical examination and tests is utilized to make a diagnosis of Graves' disease.
What Are The Treatments For Graves' Disease?
There are Three Treatments for Graves' Disease
Antithyroid Medication
Your doctor will likely prescribe you a medication to control your hyperthyroidism. There are two medications which are commonly prescribed to control hyperthyroidism. The first is methimazole and the second is propylthiouracil (PTU). These drugs prevent the thyroid from making thyroid hormone. These medications need to be prescribed by endocrinologists that understand how these medications work and potential side effects and complications from their use. These drugs usually take several weeks to work. These medications are generally not used long term for the management of Graves' disease. They are much more commonly thought of as a "short term solution". The hyperthyroidism will generally return following the stopping of either of these two medications.
There are several side effects that you should be aware of in antithyroid medications. You may develop allergic reaction to these medications. Additionally, nausea, vomiting, heart burn, metallic taste, loss of taste, and bone and muscle aches may occur. A rare condition of loss of white blood cells in the body can occur as well and must be monitored for with these medications. This condition is called agranulocytosis. If you develop fever, cough, or cold symptoms while on these medications, contact your endocrinologist immediately. It can be very serious.
These medications can be utilized to prepare you for:
- Radioactive iodine therapy
- Surgery
Radioactive Iodine Therapy
Often your doctor may favor radioactive iodine therapy more than antithyroid medication because these drugs do not produce a long term solution to the Graves' disease. The radioactive iodine is given to you in a capsule or pill type form. The radioactive iodine therapy may take months to actually produce the desired effect. Repeated treatments of radioactive iodine may be required to ultimately control Graves' disease in up to 70% of patients. Radioactive iodine is generally not sought as a therapeutic option if the patient has eye or orbital changes as a result of their Graves' disease.
Radioactive iodine is taken up by the thyroid cells that produce thyroid hormone. Because the Graves' disease thyroid cells are being "tricked" to produce more and more thyroid hormone, the radioactive iodine is taken into the thyroid hormone producing thyroid cells and a radiation effect is produced.
How much radioactive iodine is recommended for the treatment of a patient with Graves' disease is a current matter of debate.
In theory, the goal of radioactive iodine for Graves' disease is to give enough iodine to effectively treat the Graves' disease and still maintain adequate thyroid hormone production by the remaining thyroid cells. However, in most circumstances, most Graves' disease patients treated with radioactive iodine will eventually develop low thyroid hormone production (hypothyroidism) and therefore require thyroid hormone replacement long term.
If you are pregnant or plan on becoming pregnant within one year, radioactive iodine therapy should not be used.
Surgery
Surgery may be recommended for many reasons:
- Surgery is 100% effective therapy for Graves' disease
- When the Graves' thyroid gland is very large, thyroid surgery is generally considered the preferred treatment
- When antithyroid medication and radioactive iodine may be ineffective
- Some patients cannot take or tolerate antithyroid medication and radioactive iodine
- Surgery requires a total thyroidectomy
- Graves' disease surgery should only be performed by highly expert thyroid surgeons. An occastional thyroid surgeon should not do this surgery.
- If you have orbital disease, surgery is the preferred therapy for managing the Graves' disease thyroid gland.
- Requires life long thyroid hormone medications and monitoring following surgery.